What Causes Acne? The Science Behind Breakouts and the Foods That Trigger Them
You remember the first one. That stubborn red spot that appeared overnight—on your chin, your forehead, or right along your jawline—at the most inconvenient moment possible. You were told not to worry, that you’d grow out of it.
But many of us didn’t. And for a growing number of women, acne doesn’t even begin until adulthood—arriving in their 20s, 30s, or beyond. If this resonates with you, you’re not alone. Acne affects over 80% of adolescents but also persists for 64% of people in their 20s and 43% of those in their 30s— with adult women experiencing higher rates than men at every age past puberty.
Yet despite how extraordinarily common it is, most people treat acne without ever understanding what actually causes it. They chase symptoms without addressing the biology happening beneath the surface. And that, more often than not, is why the breakouts keep coming back.
Here at Natural Beauty Regimen, real results begin with understanding. In this guide, you will discover:
- The biological structure where every single breakout originates
- A surprising evolutionary reason why humans are the only species that gets acne
- The 4 root processes that transform a normal pore into an inflamed lesion
- Striking evidence that acne is not an inevitable part of life
- The specific foods that trigger breakouts — and the hormonal science behind them
Whether you are navigating your first breakouts or have been managing acne for decades, understanding its root causes changes everything. Let’s begin with the basics.


What Is Acne? More Than Just a Pimple
Acne is one of the most misunderstood conditions in skincare. It is not a hygiene problem, not a sign of laziness, and not something you simply have to endure. Acne is a chronic inflammatory disease — one with a specific biological origin, a well-documented set of causes, and, importantly, real solutions.
Clinically, acne originates in the pilosebaceous unit—a microscopic structure in your skin consisting of a hair follicle and its attached sebaceous (oil) gland. When this unit becomes disrupted, it produces the full spectrum of lesions most of us know all too well: comedones (the blackheads and whiteheads that form when pores become clogged), papules and pustules (the red, inflamed bumps and pus-filled spots), and, in more severe cases, nodules and cysts—the deep, painful lesions most likely to leave lasting scars.
Acne appears predominantly on the face, neck, chest, upper back, and shoulders—the areas of the body where pilosebaceous units are most densely concentrated. This is not a coincidence. It is biology, and we will explain exactly why in the next section.
What makes acne particularly challenging is its psychological weight. Studies consistently show that acne has a significant impact on self-confidence, social interaction, and emotional well-being—with suicidal ideation reported in 6–7% of acne patients, a figure that puts the true burden of this condition in stark perspective. So, if breakouts have ever made you want to cancel plans or avoid the mirror, that response is completely valid and entirely human.
Understanding what is actually happening inside your skin is where the path to clearer skin truly begins.
The Birthplace of Every Breakout: The Pilosebaceous Unit
To understand why acne happens, you need to understand where it happens—and that starts with a tiny structure you have never seen called the pilosebaceous unit.
Every pilosebaceous unit consists of four components: a hair shaft, a hair follicle, a sebaceous (oil) gland, and a small muscle that makes hair stand on end. Together, they form the biological environment where every single breakout begins.
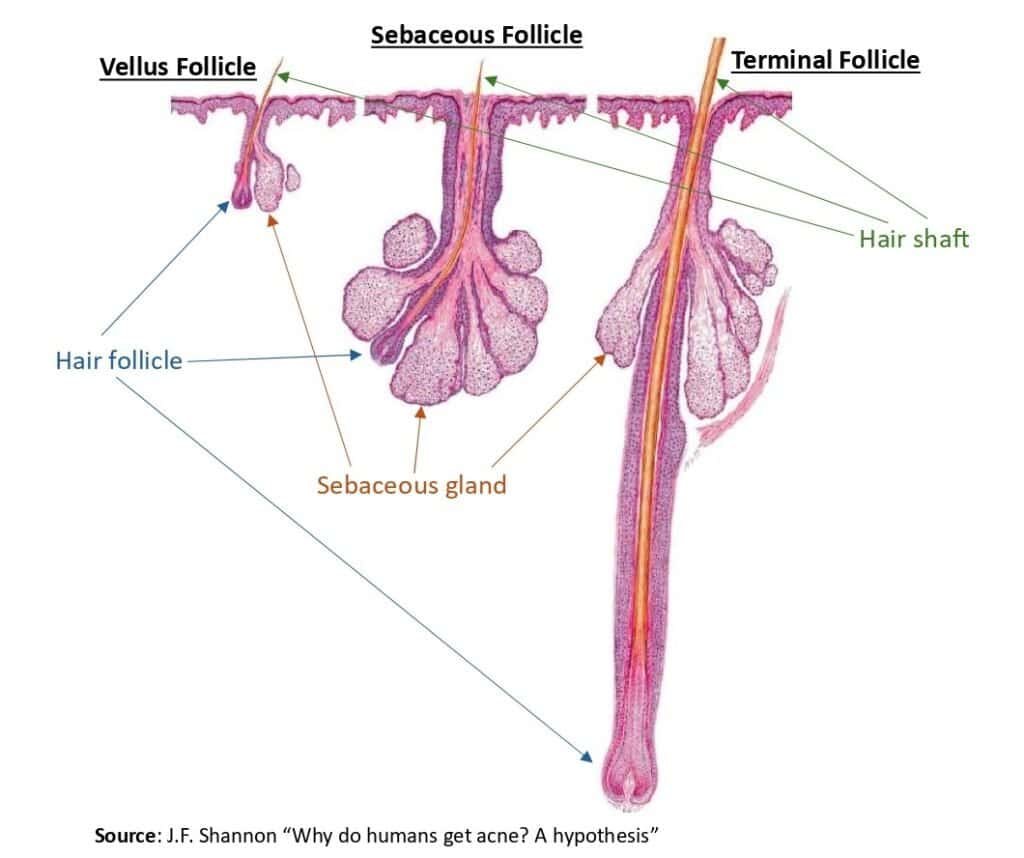
Not all pilosebaceous units are created equal, however. There are three distinct types of follicles on the face—vellus, terminal, and sebaceous— and only one of them is responsible for acne. Sebaceous follicles are uniquely vulnerable: they house an unusually large, multi-lobulated oil gland connected to a canal that is wide and deep yet carries only a tiny, wispy vellus hair. That hair is far too small to move sebum out of the follicle efficiently—meaning oil, dead skin cells, and bacteria can accumulate with nothing to clear them out. This arrangement is the perfect anatomical setup for a breakout.
What makes the face particularly susceptible is sheer density. Sebaceous follicles are packed at approximately 800 glands per square centimeter on the forehead and face—compared to just 50 per square centimeter on the arms, and zero on the palms and soles, which never develop acne. The upper back falls somewhere in between, which explains why acne there is common in more severe cases.
This is not random. The extraordinary concentration of those glands on the human face has a remarkable biological reason that has nothing to do with skincare. That reason is the subject of our next section.
Why Only Humans Get Acne: An Evolutionary Hypothesis
Here is a fact that rarely appears in skincare articles: except for minor forms in dogs and cats, acne does not occur spontaneously in any other animal on Earth. Only humans get acne. And yet, we almost never ask the most obvious question—why?
If sebaceous glands are so prone to causing problems, why has evolution kept them so extraordinarily large and dense, specifically on our faces? What purpose could possibly justify that trade-off?
The answer lies in one of the most dangerous moments in human biology: childbirth.
The human birth canal is uniquely narrow relative to the size of a baby’s head—a condition that creates a level of birth obstruction, called “dystocia,” that no other species faces to the same degree. The hypothesis, supported by compelling anatomical evidence, is that the dense concentration of sebaceous glands on a baby’s scalp, forehead, and face serves as a natural lubricant—producing high levels of sebum at birth to ease the baby’s passage through the birth canal.
The timeline supports this theory precisely. Sebaceous glands develop after the fourth month of gestation and are large and fully active at birth, driven by maternal hormones crossing the placenta. They then shrink during childhood, only to reactivate powerfully at puberty when androgens surge once more.
This is the evolutionary trade-off written into every human face: the same selective pressure that kept these glands large and numerous—generation after generation of difficult births—is the very reason our skin is vulnerable to acne when those glands are overstimulated later in life.
All humans carry this biological inheritance equally. Whether or not those sebaceous glands trigger acne depends almost entirely on the environment and diet that activates them — which is exactly what the science of breakouts reveals.
The 4 Root Causes of Acne: What’s Actually Happening Inside Your Skin
Acne is not caused by one thing. It is the result of four interconnected biological processes unfolding simultaneously inside the pilosebaceous unit. Understanding each one changes not just how you think about acne—but how you approach treating it.


Root Cause #1: Excess Sebum Production
Every breakout begins with an oil: sebum. Sebum is a mix of fats and oils made by the sebaceous gland that is constantly produced and released into hair follicle canals. In healthy amounts, it protects and hydrates the skin. In excess, it becomes, as researchers have aptly described it, the fuel for the fire of acne.
What drives overproduction? Primarily androgens—hormones like testosterone and dihydrotestosterone (DHT) that stimulate the sebaceous gland to produce more sebum and grow more active. Androgen receptors are especially concentrated in facial skin, which is why the face is ground zero for most breakouts. Puberty triggers a surge in androgens, explaining why acne so often begins in adolescence — but hormonal fluctuations throughout adulthood, particularly in women, can keep sebum overproduction going for decades.
People with acne-prone skin don’t just produce more sebum—they produce different sebum. Research shows it contains higher levels of squalene and lower levels of linoleic acid, a composition that makes it more inflammatory and more likely to clog pores.
One important nuance: most people with acne have completely normal hormone levels in their blood work. The issue is not a systemic hormonal disorder — it is a heightened local sensitivity in the sebaceous glands themselves. The glands are simply more reactive to normal androgen levels than they should be.
Root Cause #2: Follicular Hyperkeratinization — The Clogged Pore
As sebum production rises, a second process quietly prepares the ground for every visible lesion: the pore starts to clog from within.
In healthy skin, keratinocytes—the cells lining the inside of the follicular canal— shed regularly and exit through the pore opening. In acne-prone skin, this shedding process breaks down. Keratinocytes multiply quicker than they fall off, building up inside the canal with extra sebum until the pilosebaceous unit gets blocked.
This obstruction is called a microcomedo—an invisible blockage that is the precursor to every single acne lesion you have ever seen. As the microcomedo grows, it becomes a visible closed comedone (whitehead) if the pore remains sealed or an open comedone (blackhead) if the pore is open and the trapped sebum oxidizes on contact with air. The dark color of a blackhead is not dirt — it is oxidized melanin.
Crucially, research now shows that inflammation begins at this stage — before the lesion is even visible. The immune signal IL-1α plays a key role in triggering comedone formation, meaning acne is an inflammatory disease from its earliest moments, not just in its later, angrier stages.
The reason sebaceous follicles are so much more vulnerable to this process than terminal follicles goes back to what we established in Section 2: the tiny vellus hair attached to the sebaceous follicle cannot wick sebum outward the way a thick terminal hair does on the scalp. Without that mechanical clearing, obstruction is almost inevitable when sebum production rises.
Root Cause #3: C. acnes Colonization
Once the follicle is blocked and filling with sebum, a third player enters: Cutibacterium acnes—formerly known as Propionibacterium acnes and commonly referred to as C. acnes.
C. acnes is not a foreign invader. It lives on everyone’s skin as part of the normal microbiome. It thrives in sebum-rich, low-oxygen environments—which means a blocked, sebum-filled follicle is its ideal habitat. As it colonizes the trapped contents of the microcomedo, it releases enzymes called lipases that break down triglycerides in sebum into free fatty acids. Those free fatty acids are directly inflammatory to the surrounding tissue.
C. acnes also can form biofilms — structured colonies that adhere to the follicular wall and are significantly more resistant to antibiotics than free-floating bacteria. This is one reason why antibiotic treatments for acne can lose effectiveness over time.One important clarification: C. acnes alone does not cause acne. The number of C. acnes bacteria on the skin does not correlate with acne severity — people with clear skin carry it too. It is better understood as an amplifier of the inflammatory process rather than the root cause. Remove the blocked follicle and the excess sebum, and C. acnes has nowhere to thrive.
Root Cause #4: The Inflammatory Response
The final and most visible phase of acne is inflammation—and it is this response that determines exactly what kind of lesion appears on your skin.
When C. acnes affects the hair follicle area, it activates the immune system using a receptor called “Toll-like receptor 2” (TLR-2), which starts a series of inflammatory signals like IL-1α, IL-8, and TNF-α. These signals recruit neutrophils, macrophages, and lymphocytes to the site. What follows is a targeted immune assault on the blocked follicle.
The nature of that assault determines the lesion:
- A mild, contained response produces a papule—a small, firm red bump
- A more intense response drives fluid and immune cells to the surface, forming a pustule.
- A deep, severe inflammatory response creates nodules or cysts—the painful, deep lesions most associated with scarring
When inflammation is severe enough to rupture the follicular wall, the contents spill into the surrounding dermis. The immune system, treating sebum and keratin debris as foreign material, mounts an even broader response — spreading inflammation through deeper layers of skin and significantly raising the risk of permanent scarring.
These four processes — excess sebum, clogged pores, bacterial colonization, and inflammation — do not happen in a neat sequence. They are simultaneous, mutually reinforcing, and cyclical. But here is the critical question they raise: what sets this entire cascade in motion in the first place? The evidence, drawn from some of the most striking population-level research in dermatology, points directly to lifestyle—and most powerfully, to diet.
Acne Is Not Inevitable: What Two Isolated Populations Teach Us
Everything we have covered so far—the sebaceous glands, the four root causes, and the inflammatory cascade— exists in every human body on the planet. Every person who has ever gone through puberty carries the same biological inheritance. So why do some populations develop no acne at all?
The answer comes from two landmark studies that quietly changed how dermatologists think about acne.
The first population studied was the Kitavan Islanders of Papua New Guinea — a community of 1,200 people living as subsistence farmers and fishermen, largely untouched by Western food systems. Over seven weeks, a physician trained in acne diagnosis examined every resident, including 300 people aged 15 to 25 — the highest-risk window for acne development. The finding was extraordinary: the entire population showed no signs of papules, pustules, or open comedones. Zero cases of acne. In a Western population of the same size and age, researchers would expect at least 120 people to show visible acne.
The second population was the Ache hunter-gatherers of Paraguay, observed continuously over 843 days by seven trained physicians. Among all the 115 subjects examined—including teenagers and young adults— not a single case of acne vulgaris was recorded.
These are not genetic anomalies. Related South American and Pacific Islander populations living in Westernized settings develop acne at rates comparable to Western societies. When the same ethnic groups adopt a Western lifestyle, acne follows. The difference is entirely environmental.
Both populations share two defining dietary characteristics: they eat minimally processed whole foods, and they consume virtually no refined carbohydrates, dairy, or sugar. Both groups also maintain strikingly low insulin levels throughout their lives.The conclusion is difficult to escape: acne is not an inevitable consequence of puberty or human biology. It is, in significant part, a disease of the modern Western diet.
The Foods That Trigger Acne Breakouts — And the Science Behind Them
Diet influences acne through one central pathway: hormonal and inflammatory signaling. The foods that cause the most damage are those that spike insulin, elevate IGF-1, or introduce exogenous hormones into the body—all of which feed directly into the four root causes we explored earlier. Understanding this mechanism transforms the way you contemplate what you eat and what appears on your skin.


Trigger #1: High Glycemic Foods — Why Glycemic Load Matters More Than Glycemic Index
When it comes to diet and acne, you have probably heard that high-glycemic foods are a problem. But there is an important distinction that most articles skip over—one that could be causing you to unnecessarily avoid perfectly healthy foods while missing the ones that are actually driving your breakouts.
What Is the Glycemic Index?
The glycemic index (GI) measures how quickly a specific food raises blood sugar compared to pure glucose. Foods are ranked on a scale of 0 to 100 — the higher the number, the faster the blood sugar spike. White bread scores around 70. Table sugar scores 65. Jelly beans score 80.
The problem with GI alone is that it only tells you how fast a food raises blood sugar—not how much it actually raises it in a realistic portion. And that distinction matters enormously for your skin.
Why Glycemic Load Is the More Important Metric
Glycemic load (GL) corrects this gap by accounting for both the speed and the quantity of carbohydrates actually delivered per serving. The formula is straightforward: GL = GI × grams of carbohydrate per serving ÷ 100.
Consider watermelon. Its GI is approximately 72—technically high, placing it in the same category as white bread. Yet a standard serving of watermelon is over 90% water and delivers very few digestible carbohydrates, giving it a GL of just 5—firmly in the low range. Eating watermelon does not meaningfully spike insulin. Avoiding it because of its GI score alone would be an unnecessary and scientifically unfounded restriction.
Now consider a bowl of cornflakes. Its GI is 84—high. But unlike watermelon, a standard serving delivers a dense carbohydrate load, resulting in a GL of 73. This is a food that truly and significantly increases insulin levels, making it worthy of your attention.
Glycemic load is the metric that reflects what actually happens hormonally after a real meal. It is the number that matters for your skin.
The Hormonal Cascade That Connects High-GL Foods to Acne
Here is why high-GL foods are so problematic for acne-prone skin. A high-GL meal causes a rapid spike in blood glucose, which triggers a surge in insulin. That insulin surge stimulates the production of insulin-like growth factor 1 (IGF-1), a hormone that drives sebocyte proliferation, meaning more oil-producing cells generating more sebum. IGF-1 simultaneously accelerates follicular hyperkeratinization—the very pore-clogging process we described in Root Cause #2.
Insulin also suppresses sex hormone-binding globulin (SHBG), the protein that keeps androgens in check— leaving more free testosterone circulating in the blood and further stimulating sebaceous gland activity. The result is a hormonal environment that feeds every single one of the four root causes of acne simultaneously.
Underlying all of these changes is a nutrient-sensing pathway called mTORC1—overactivated by high-GL diets and directly responsible for driving sebaceous gland proliferation and keratinocyte growth. Some researchers now classify acne alongside obesity, type 2 diabetes, and certain cancers as an mTORC1-driven disease of Western civilization—a term that reflects just how fundamentally diet shapes this condition at the cellular level.
The High-GL Foods Most Strongly Linked to Acne
With glycemic load as our lens, the foods that most reliably drive the acne-triggering hormonal cascade are:
- Refined grain products: white bread, bagels, white rice, pasta made from refined flour, crackers
- Breakfast cereals: most commercial cereals, including those marketed as healthy
- Sugary drinks: sodas, fruit juices, energy drinks, sweetened coffees
- Processed snacks: chips, cookies, pastries, candy bars, doughnuts
- Added sugars in any form: table sugar, high-fructose corn syrup, syrups
The contrast with the Kitavan and Ache diets could not be sharper. Both populations consumed approximately 70% of their daily calories from carbohydrates—yet developed zero acne. Their carbohydrate sources were exclusively low-GL: tubers, whole fruits, and vegetables. Their carbohydrate intake was high; their glycemic load—and their insulin response—was low. Multiple randomized controlled trials confirm that switching to a low-GL diet produces measurable, significant reductions in acne severity.
The takeaway is not to fear carbohydrates. It is to choose ones that your body processes gradually—and to be clear-eyed about the ones that do not.
Trigger #2: Dairy Products — A Different Mechanism, an Equal Impact
The previous section established that high-GL foods drive acne primarily by spiking insulin. Dairy adds a significant and insightful complexity to this issue — the problem with dairy is not its glycemic load.
Milk actually has a relatively low GL. By that metric alone, it should be harmless for your skin. Yet multiple observational studies across diverse populations consistently link cow’s milk consumption to increased acne risk and severity. Understanding why requires looking beyond glycemic load entirely—and into dairy’s unique hormonal and protein profile.
Why Dairy Is a Special Case
Cow’s milk is biologically engineered to grow a calf rapidly. It naturally contains IGF-1, androgens, and other growth-signaling hormones that remain biologically active after human consumption, interacting directly with the same receptors that drive sebum production and follicular clogging.
Beyond its hormonal content, both whey and casein—the two primary proteins in milk— independently stimulate a disproportionately high insulin response, entirely separate from any carbohydrate content. Whey in particular produces an insulin spike that rivals high-GL foods, feeding the exact same hormonal cascade we described in Trigger #1—elevated IGF-1, suppressed SHBG, and increased free androgens—without a single gram of refined carbohydrate involved.
This means dairy and high-GL foods can act as independent but additive triggers. A breakfast of cornflakes with skim milk combines both pathways simultaneously—a high-GL carbohydrate load on top of whey-driven insulin stimulation—creating a hormonal environment that is particularly hostile to acne-prone skin.
The Counterintuitive Skim Milk Finding
Skim milk, more than whole milk, has been found to have the strongest acne associations among dairy products, which contradicts most people’s intuitions. The likely explanation is twofold: removing fat alters the hormonal bioavailability of milk proteins, and skim milk is frequently supplemented with additional whey protein concentrate during processing to improve texture, further amplifying its insulin-stimulating effect.
Cheese appears to carry a weaker association, possibly because fermentation processes alter its protein and hormonal profile significantly. Ice cream, interestingly, shows a stronger association — likely because it combines dairy’s hormonal payload with a high sugar content, stacking both acne triggers at once.
The evidence here remains largely observational rather than from controlled trials. But it is consistent across independent studies conducted in different countries, age groups, and ethnicities—making it difficult to dismiss. If your skin reliably worsens with dairy consumption, that pattern is almost certainly real and scientifically grounded.
What to Eat Instead: Building an Anti-Acne Plate
Now that we have established what drives breakouts from the inside—high-GL foods spiking insulin through carbohydrate overload and dairy spiking it through protein and hormonal pathways—the more empowering question becomes: what should you be eating more of?
This is not about following a rigid acne elimination diet. It is about building eating habits that keep your insulin response stable, your androgens in check, and your skin’s inflammatory burden low.


Prioritize Low-GL Carbohydrates
The most impactful dietary shift you can make is replacing high-GL foods with low-GL alternatives that deliver steady, gradual energy without triggering the hormonal cascade. Think vegetables, legumes, whole fruits, sweet potatoes, oats, brown rice, and whole-grain products. Importantly—as the watermelon example illustrated—this approach does not mean avoiding fruit. Most whole fruits have a low GL despite their natural sweetness, and their fiber content further slows glucose absorption.
Fiber deserves special mention here. Beyond its role in slowing carbohydrate digestion, fiber feeds a healthy gut microbiome—increasingly recognized as a key player in skin health through what researchers call the gut-skin axis. High-GL diets disrupt gut bacteria balance, increase intestinal permeability, and allow pro-inflammatory molecules to enter the bloodstream and reach the skin. A fiber-rich, low-GL diet does the opposite, addressing acne from both the hormonal and inflammatory angles simultaneously.
Add Omega-3 Rich Foods
Omega-3 fatty acids — found in fatty fish like salmon and sardines, walnuts, flaxseeds, and chia seeds — directly modulate the inflammatory pathways involved in acne at the follicular level. Where high-GL foods and dairy ignite the acne cascade, omega-3s help dampen it.Think of the dietary strategy in two complementary layers: removing high-GL foods and dairy reduces the hormonal signals that start the breakout cycle. Adding omega-3s and fiber-rich whole foods reduces the inflammatory response that escalates it. Both matter—and together, they represent the most evidence-backed nutritional approach to clearer skin available today.
Other Factors That Can Trigger or Worsen Acne
Diet is one of the most powerful levers for managing acne. But for many people, especially adult women, several non-dietary triggers operate quietly in the background, making breakouts more frequent, more severe, or more resistant to improvement.
Hormonal fluctuations are often the most significant. The menstrual cycle creates predictable shifts in estrogen and progesterone that directly influence sebum production—explaining the reliable pre-period breakout many women know well. Conditions like PCOS, perimenopause, pregnancy, and hormonal contraceptives all shift the hormonal environment in ways that keep sebaceous glands overstimulated. As established in Root Cause #1, the issue is rarely abnormal hormone levels — it is the local sensitivity of the sebaceous glands to normal fluctuations. That sensitivity does not show up on a blood test, but it shows up on your skin.
Stress does not cause acne, but it reliably worsens it. Cortisol stimulates adrenal androgen production, raises systemic inflammation, and lowers the threshold at which a contained papule escalates into something deeper and angrier. It also shifts behavior—more face-touching, disrupted sleep, and a pull toward high-GL comfort foods—compounding the effect through multiple pathways simultaneously.
Genetics sets your baseline reactivity—how sensitive your sebaceous glands are to androgens and how intense your inflammatory response runs. It does not determine your outcome, as the Kitavan and Ache evidence makes clear, but it does explain why two people with identical diets can have completely unique skin.
Comedogenic skincare and makeup products can physically initiate microcomedo formation from the outside in, independently of any hormonal trigger—a frequently overlooked variable that we explore fully in our upcoming guide to The Best Skincare Routine for Acne-Prone Skin.
Conclusion: Understanding Acne Is the First Step to Clearing It
Every breakout you have ever experienced traces back to the same origin: a pilosebaceous unit pushed beyond its threshold by a combination of excess sebum, a clogged follicle, bacterial activity, and inflammation. Those four processes are biological. Your choices largely influence what sets these processes in motion and how intensely they fire.
The evidence from the Kitavan Islanders and the Ache hunter-gatherers is not a niche footnote. This is a key finding in modern dermatology, as it confirms that acne is not an inevitable result of having human skin. It is a disease with identifiable triggers, and those triggers can be addressed.
Reducing high-GL foods and dairy removes the hormonal fuel that ignites the cascade. Managing stress, understanding your hormonal patterns, and auditing your skincare products address the triggers that sustain it. None of this requires perfection — it requires awareness. And awareness begins exactly where you are right now.
At Natural Beauty Regimen, we believe that understanding your skin is the foundation of caring for it well. This post is the first in a series designed to give you that foundation, layer by layer.
Now that you understand what causes acne and why, the next question is, Which ingredients actually have the power to treat and prevent it? We explore that in depth in our next guide:
➡ 8 Botanical Ingredients That Help Treat and Prevent Acne
And once you know the ingredients, how do you build them into a routine that actually works?
➡ The Best Skincare Routine for Acne-Prone Skin (Step by Step)
Understanding your skin is the first step toward clearing it. You have just taken it.
Other Posts You May Like:
- The Best Skincare Routine for Acne-Prone Skin (Step by Step)
- 8 Botanical Ingredients That Help Treat and Prevent Acne
- 6 Proven Skin Benefits of Polypodium Leucotomos Backed by Science.
- How to Use Niacinamide for Best Results
- 7 Niacinamide Benefits for Skin Care
- 9 Best Polypodium Leucotomos Supplements for Sun Protection & Glowing Skin
- The Truth About Sunscreen: 8 Facts The Industry Doesn’t Want You To Know
- Natural Skincare Routine for Hyperpigmentation: A Step-by-Step Guide
- How to Treat Hyperpigmentation Naturally: A Complete Guide





